Diabetic retinopathy — vision-threatening damage to the retina of the eye caused by diabetes — is the leading cause of blindness among working-age Americans, according to the U.S. National Institutes of Health (NIH).
Yet, many cases could be prevented with regular eye exams and appropriate treatment.
According to a report released by the International Diabetes Federation (IDF) at the World Diabetes Congress held in Vancouver in December 2015, the United States has the highest rate of diabetes among 38 developed nations, with approximately 30 million Americans — roughly 11 percent of the U.S. population between the ages of 20 and 79 — having the disease.
About 90 percent of Americans with diabetes have type 2 diabetes, which develops when the body fails to produce enough insulin — a hormone secreted by the pancreas that enables dietary sugar to enter the cells of the body — or the body becomes resistant to insulin. This causes glucose (sugar) levels in the bloodstream to rise and can eventually damage the eyes, kidneys, nerves, or heart, according to the American Diabetes Association (ADA).
Risk factors for type 2 diabetes include obesity, an unhealthful diet, and physical inactivity. Unfortunately, the prevalence of obesity and type 2 diabetes has increased significantly in the United States over the past 30 years.

In the late stages of diabetic retinopathy, you may have blind spots and/or floaters.
According to data released by the U.S. Centers for Disease Control and Prevention (CDC) in December 2015, there were 1.4 million new cases of diabetes reported in the U.S. in 2014. Though this annual number is down from the historic high of 1.7 million new cases in 2009, it is still three times higher than what it was in 1980.
Between 12,000 and 24,000 new cases of blindness from diabetic retinopathy occur in the United States each year, according to CDC, and many could be prevented with early intervention. But a significant percentage of Americans with diabetes are not aware of their risk of vision impairment from the disease.
In November 2015, Regeneron Pharmaceuticals reported the results of a survey conducted for the company by the Market Research Group at Everyday Health that revealed less than half of adults with diabetes in the U.S. recognize their risk for vision loss.
The survey results also showed that only 18 percent of respondents were familiar with diabetic macular edema (DME), a term that refers to the swelling of the macula associated with diabetic retinopathy, and nearly one third (30 percent) of respondents said they don’t get annual dilated eye exams recommended by the National Eye Institute for people with diabetes, which could help protect against diabetes-related vision loss.
People who are most vulnerable to diabetic retinopathy, including the elderly and certain minorities, may not receive appropriate eye care because of a lack of health insurance or access even to primary care physicians.
For these reasons, make sure you promptly advocate for your own eye health and that of affected family members or friends when any kind of diabetes is present.
Generally, diabetics don’t develop diabetic retinopathy until they have had diabetes for at least 10 years. But it is unwise to wait that long for an eye exam.
With any diagnosis of diabetes, your primary care physician should refer you to an optometrist or ophthalmologist who will give you a dilated eye exam at least once a year.
How Does Diabetes Cause Diabetic Retinopathy?
Diabetes mellitus (DM) causes abnormal changes in the blood sugar (glucose) that your body ordinarily converts into energy to fuel different bodily functions.
Uncontrolled diabetes allows unusually high levels of blood sugar (hyperglycemia) to accumulate in blood vessels, causing damage that hampers or alters blood flow to your body’s organs — including your eyes.
Diabetes generally is classified into two types:
- Type 1 diabetes. Insulin is a natural hormone that helps regulate the levels of blood sugar needed to help “feed” your body. When you are diagnosed with type 1 diabetes, you are considered insulin-dependent because you will need injections or other medications to supply the insulin your body is unable to produce on its own. When you don’t produce enough of your own insulin, your blood sugar is unregulated and levels are too high.
- Type 2 diabetes. When you are diagnosed with type 2 diabetes, you generally are considered non-insulin-dependent or insulin-resistant. With this type of diabetes, you produce enough insulin but your body is unable to make proper use of it. Your body then compensates by producing even more insulin, which can cause an accompanying abnormal increase in blood sugar levels.
With both types of diabetes, abnormal spikes in blood sugar increase your risk of diabetic retinopathy.
Eye damage occurs when chronically high amounts of blood sugar begin to clog or damage blood vessels within the eye’s retina, which contains light-sensitive cells (photoreceptors) necessary for good vision.
Symptoms Of Diabetic Retinopathy And Other Diabetes-Related Eye Problems
You first may notice diabetic retinopathy (DR) or other eye problems related to diabetes when you have symptoms such as:
- Fluctuating vision
- Eye floaters and spots
- Development of a scotoma or shadow in your field of view
- Blurry and/or distorted vision
- Corneal abnormalities such as slow healing of wounds due to corneal abrasions
- Double vision
- Eye pain
- Near vision problems unrelated to presbyopia
- Cataracts
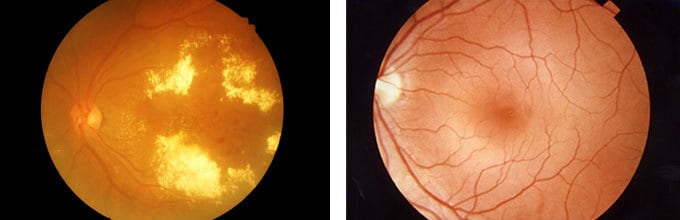
Background diabetic retinopathy (top image) is an early sign of damage to the retina at the back of the eye, where blood vessels begin to weaken and leak. The leakage causes accumulations of yellowish proteins and fatty substances. Compare that with the appearance of a healthy eye (bottom image: National Eye Institute, National Institutes of Health).
During an eye examination, your eye doctor will look for other signs of diabetic retinopathy and diabetic eye disease. Signs of eye damage found in the retina can include swelling, deposits and evidence of bleeding or leakage of fluids from blood vessels.
For a definitive diagnosis, you may need to undergo a test called a fluorescein angiography. In this test, illuminated dye is injected into the body through your veins (IV). As your blood flows, the dye gradually appears in the retina.
Your ophthalmologist will photograph the retina and evaluate its appearance with the help of the illuminated dye. This analysis helps determine if the disease is present and how far it has progressed.
One sometimes overlooked symptom of diabetic eye disease is nerve damage (neuropathy) affecting ocular muscles that control eye movements. Symptoms can include involuntary eye movement (nystagmus) and double vision.
Types Of Diabetic Eye Disease
Once high blood sugar damages blood vessels in the retina, they can leak fluid or bleed. This causes the retina to swell and form deposits in early stages of diabetic retinopathy.
In later stages, leakage from blood vessels into the eye’s clear, jelly-like vitreous can cause serious vision problems and eventually lead to blindness.
Clinically significant macular edema (CSME). This swelling of the macula more commonly is associated with type 2 diabetes. Macular edema may cause reduced or distorted vision.
Diabetic macular edema (DME) typically is classified in two ways:
- Focal, caused by microaneurysms or other vascular abnormalities sometimes accompanied by leaky blood vessels.
- Diffuse, which describes dilated or swollen tiny blood vessels (capillaries) within the retina.
If you have CSME, you typically are advised to undergo laser photocoagulation.
Non-proliferative diabetic retinopathy (NPDR). This early stage of DR — identified by deposits forming in the retina — can occur at any time after the onset of diabetes.
Often no visual symptoms are present, but examination of the retina can reveal tiny dot and blot hemorrhages known as microaneurysms, which are a type of out-pouching of tiny blood vessels.
In type 1 diabetes, these early symptoms rarely are present earlier than three to four years after diagnosis. In type 2 diabetes, NPDR can be present even upon diagnosis.
Proliferative diabetic retinopathy (PDR). Of the diabetic eye diseases, proliferative diabetic retinopathy has the greatest risk of visual loss.
The condition is characterized by these signs:
- Development of abnormal blood vessels (neovascularization) on or adjacent to the optic nerve and vitreous.
- Pre-retinal hemorrhage, which occurs in the vitreous humor or front of the retina.
- Ischemia from decreased or blocked blood flow, with an accompanying lack of oxygen needed for a healthy retina.
These abnormal blood vessels formed from neovascularization tend to break and bleed into the vitreous humor of the eye. Besides sudden vision loss, more permanent complications can include tractional retinal detachment and neovascular glaucoma.
Macular edema may occur separately from or in addition to NPDR or PDR.
You should be monitored regularly, but you typically don’t require laser treatment for diabetic eye disease until the condition is advanced.
Who Gets Diabetic Retinopathy?
Beyond the presence of diabetes, how well your blood sugar is controlled is a major factor determining how likely you are to develop diabetic retinopathy with accompanying vision loss.
Uncontrolled high blood pressure (hypertension) has been associated with eye damage related to diabetes. Also, studies have shown a greater rate of progression of diabetic retinopathy in diabetic women when they become pregnant.
Of course, the longer you have diabetes the more likely you are to have vision loss.
The American Academy of Ophthalmology (AAO) notes that all diabetics who have the disease long enough eventually will develop at least some degree of diabetic retinopathy, though less advanced forms of the eye disease may not lead to vision loss.
Minorities And Diabetic Retinopathy
In the United States, minorities appear particularly vulnerable to vision loss caused by diabetic eye disease.
In early 2010, U.S. House Majority Whip James E. Clyburn, D-SC, noted that diabetic retinopathy is now an epidemic among African-Americans older than age 20.
“People with diabetes are 25 times more likely to go blind, and African-Americans with diabetes are at an even higher risk — almost 50 percent more likely to develop diabetic retinopathy,” Clyburn said in an announcement sponsored by the AAO and the American Diabetes Association.
Hispanics with diabetes also are at higher risk of developing diabetic retinopathy and vision loss.
Los Angeles Latino Eye Study results announced in May 2010 show that 42 percent of Hispanics who have had diabetes for more than 15 years also will develop diabetic retinopathy, compared with a general population average of 15 percent.
The study, sponsored by the National Eye Institute, found that Hispanics were more likely to develop diabetic retinopathy than non-Hispanic Caucasians.
“These results underscore the importance of Latinos, especially those with diabetes, getting regular, dilated eye exams to monitor their eye health,” said principal investigator Rohit Varma, MD, director of the Ocular Epidemiology Center at the Doheny Eye Institute, University of Southern California. “Eye care professionals should closely monitor Latinos who have eye disease in one eye because their quality of life can be dramatically impacted if they develop the condition in both eyes.”
Native Americans also are at high risk of developing diabetes and related diabetic eye disease. As an example, Pima Indians have a 35 percent prevalence of diabetes compared with 8 to 9 percent of the general U.S. population.
When Is Diabetic Retinopathy A Disability?
You must make every effort through medical intervention and other remedies to address diabetes and diabetic retinopathy before you qualify for special considerations under the Americans with Disabilities Act (ADA).
A disability basically means that you are substantially limited in the way you function in daily activity. When you are disabled, you are entitled to certain reasonable accommodations at the workplace and at public places such as schools.
ADA amendments added in 2008 further clarify that diabetics, in particular, have certain protections under the law, such as needed breaks at the workplace for insulin injections or lunches at set times to maintain blood sugar levels.
You cannot be fired from your job or denied employment strictly because you are diabetic, as long as you are able to handle the basics of your work tasks.
As an example, the American Diabetes Association says that a person with mild diabetic retinopathy easily might perform daytime tasks but could have difficulty with night vision. In this case, special accommodations such as appropriate lighting might be needed at the workplace.
If questions arise, you may need a letter from your physician that advises an employer regarding how well you will be able to perform certain work tasks. Your physician also could explain any special accommodations you might need, such as extra lighting.
State regulations governing disability differ, so you also should check guidelines established by the state in which you reside.
If you are visually impaired enough that you cannot work and expect the condition to last at least a year, you may be qualified for Social Security disability benefits.
To qualify, you previously must have been in the workforce for a length of time that depends on your age. You can contact your local Social Security representative for details or go online to view specific U.S. Social Security Administration guidelines at www.ssa.gov.
Eye Exam Assistance Program
According to the CDC, almost 27 percent of Americans age 65 or older had diabetes in 2010.
If you are 65 or older and have not seen an eye doctor in three years, you might be eligible for a free comprehensive eye exam to check for diabetic retinopathy through EyeCare America, a public service program of the Foundation of the American Academy of Ophthalmology. The program also covers up to one year of care for any eye disease detected during the exam.
Volunteer ophthalmologists participating in the EyeCare America program waive co-payments, accepting Medicare or other eye care insurance reimbursement as payment in full. If you don’t have vision insurance, the services are free.
To learn more about the EyeCare America program and see if you are eligible, visit www.EyecareAmerica.org.


